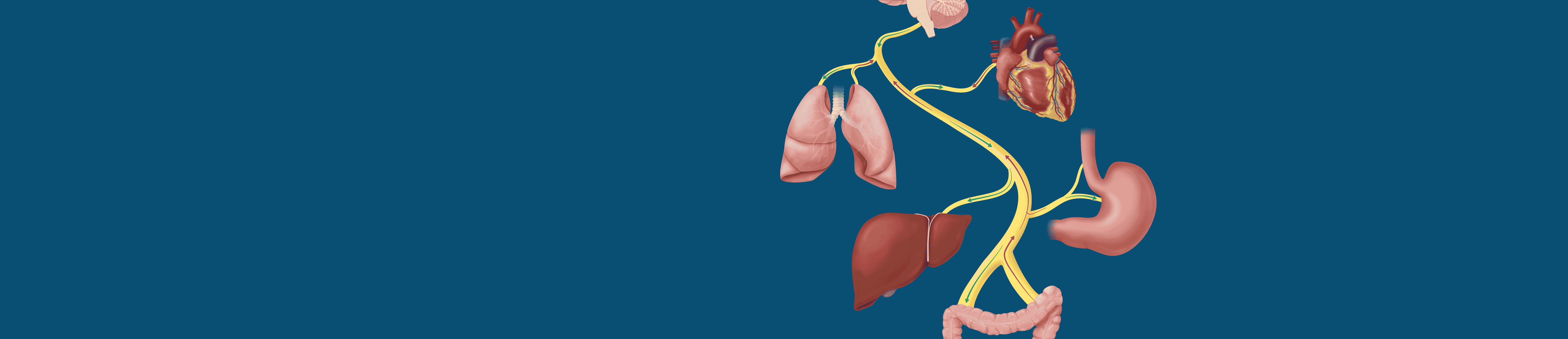
Second in length only to the sciatic nerve, our paired cranial nerve 10 arises from the brainstem, migrates through the neck and thorax, and terminates in the gut. Along its course, aptly deriving its name from Latin for the wanderer, the vagus nerve prolifically liberates its fibers to our palate, ear, larynx, pharynx, heart, lungs, and digestive system. It is thought that vagus nerve stimulation can have positive health benefits for a variety of ailments.
______________________________________________________________________________________________________________
|Table of Contents
- Why Try to Harness the Vagus Nerve?
- Noninvasive Electrical Vagal Nerve Stimulation
- Surgically Invasive Vagal Nerve Stimulation
- Does Invasive Vagus Nerve Stimulation Work in Treating Epilepsy?
- The Spawning of Noninvasive Vagus Nerve Stimulation Approaches
- How Does Vagus Nerve Stimulation Work?
- And What “Home Remedies” Are There?
______________________________________________________________________________________________________________
Why try to stimulate the vagus nerve?
Consider other words with vagus as their root: vagabond, vagrant, and vague—all have, at their core, a diffuse, rambling, not stationary connotation. The vagus nerve certainly lives up to its Latin origin.
Regarding our anesthetic management, think about the attention we devote to this mainstay of the parasympathetic side of our autonomic nervous system. We use many pharmacological interventions to keep it from provoking undesirable manifestations, including bradycardia, arrhythmias, bronchoconstriction, nausea, salivation, acid secretion, and swallowing.
We know the vagus nerves (they are paired) not as single cables but as diffuse bundles of thousands of fibers spread throughout the neck, upper torso, and abdomen. Like the branches of a tree, the fibers emerge, reaching out and contacting virtually everything in their path.
While the vagus nerve has an effect of one sort or another on virtually every organ in the body, let’s focus on what has become a focal point of the public’s fascination with how to improve overall well-being. Social media (e.g., TikTok videos viewed by tens of millions!), the healthcare community, governmental agencies, and many wellness companies invest great interest in the nerve. Several companies market the vagus nerve as promoting mood, reducing anxiety, and amping the immune system.
We want to be clear from the start: APEX has no financial ties to anything in the vagus nerve stimulation (VNS) marketplace, nor do we encourage or discourage the approaches we will examine. We mention products and techniques only to help illuminate what the landscape looks like and what conditions VNS is targeted at and marketed for.
How to stimulate the vagus nerve
There are two methods for vagus nerve stimulation: noninvasive electrical and surgical invasive stimulation. Let’s explore each of these.
Noninvasive electrical vagus nerve stimulation
Neuvana XenTM is a noninvasive, electrical pulsed, transcutaneous VNS device paired with earbuds. Mild electrical stimulation is delivered through the ear and targets the vagus nerve to reduce stress and induce relaxation. TruvagaTM is another handheld device that is strategically placed over the neck. Transcutaneous stimulation targets the vagus lying beneath the skin. Both companies report that their devices relieve anxiety, enhance clarity in thinking, improve sleep, and promote wellness. The devices are sleek and sexy in their design.
Surgically invasive vagus nerve stimulation
Your APEX crew has experience providing care for drug-resistant epilepsy patients having an implanted FDA-approved VNS. Typically, the anesthesia provider induces general anesthesia, and an ETT or LMA placement occurs. The left vagus is usually targeted as more cardiac efferents emerge from the right-sided nerve; stimulating it might result in greater cardiac rhythm effects. The surgeon attaches a lead to the exposed vagus nerve and creates a cavity for the VNS generator in the anterior left chest. A tunneling technique connects the cable affixed to the nerve with the generator. After final programming, the surgeon checks lead integrity and impedance, and completes the procedure.
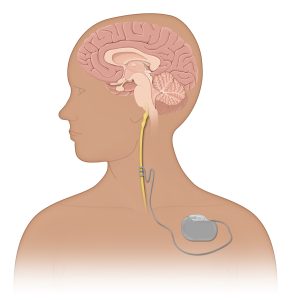
These patients are often on heavy-duty antiseizure meds. We’ve found a propofol-based technique with low-dose sevoflurane and minimal opioid (if any) works well. Management is usually routine, but always be mindful of the implications of possible surgical trauma to the trachea or the carotid artery.
Does invasive vagus nerve stimulation work in treating epilepsy?
We found recent literature demonstrating that invasive VNS has significant efficacy in treating epilepsy by either decreasing the frequency of an event or abbreviating its duration. But then came what so often does with new drugs and interventions, incidental findings!
In this case, there were frequent but anecdotal observations of mood elevation in patients who had undergone VNS for their epilepsy. We know what you’re thinking: improve the epilepsy condition with VNS, and patients will feel better. We thought so, too. But, clinical researchers wondered if more was happening, so small randomized controlled trials were conducted involving those without epilepsy suffering from depressive disorders.
Early successes suggested the need to extend treatment duration, and the RECOVER trial is now underway, where researchers will study patients for 6 years. Treatment of depression is usually a time-intensive process.
Some evidence even suggests that stimulating the vagus directly or with somatic therapy may have benefits in alleviating PTSD. Here too, the quality of evidence is just not there yet.
The spawning of noninvasive vagus nerve stimulation approaches
The FDA approved noninvasive VNS approaches for adults suffering from severe depression in 2005. Invasive VNS is expensive, logistically challenging, and carries the risks associated with surgery and anesthesia. The race was on to develop noninvasive approaches. The most efficient method and the focus of most current activity involves transcutaneously stimulating the vagus nerve’s auricular branches.
The marketplace is exploding with devices and interventions targeting not only epilepsy and diabetes but also:
- Obesity
- Cluster and migraine headaches
- Autoimmune disorders such as Crohn’s disease
- Anxiety disorders
- Alzheimer’s syndrome.
How does vagus nerve stimulation sork?
While the precise action of VNS remains inconclusive, experts in the field believe creating new action potentials activate the limbic system and generally affects brainstem arousal mechanisms. This is a complex terrain to study, and we should realize that the long-term effects of implanted devices remain foggy.
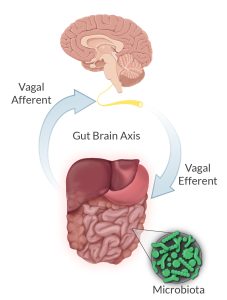
Recall that the vagus is a mixed sensory and motor nerve, with 70-80% of its fibers serving an afferent role. Research demonstrates that the vagus nerve plays an important role in the gut-brain axis, which is receiving much attention in the scientific and lay press. There is still much that we must learn.
And What “Home Remedies” Are There?
VNS’s success with medical interventionalists prompts many to seek alternative, somatic methods with plenty of wellness industry approaches. A wide range of VNS devices, oral supplements, and skin lotions that have yet to be rigorously studied are available. Anecdotal reports and testimonials fuel their pursuit.
There are reports of face submersion into very cold water, placing ice bags on the neck or chest, and contouring the neck and torso to compress and activate the vagus nerve directly. Even simpler interventions like focused deep breathing exercises, singing, humming, and loud gargling with water are advocated to stimulate the vagus nerve.
While many “home remedies” seem safe, negative anecdotes exist about vertigo, syncope, bradycardia, dyspnea, dysphagia, voice changes, and visual disturbances. A lot is happening here, so it seems reasonable to be mindful of the potential of your “wanderer.”
As CRNAs ourselves, we understand the challenge of fitting CRNA continuing education credits into your busy schedule. When you’re ready, we’re here to help.